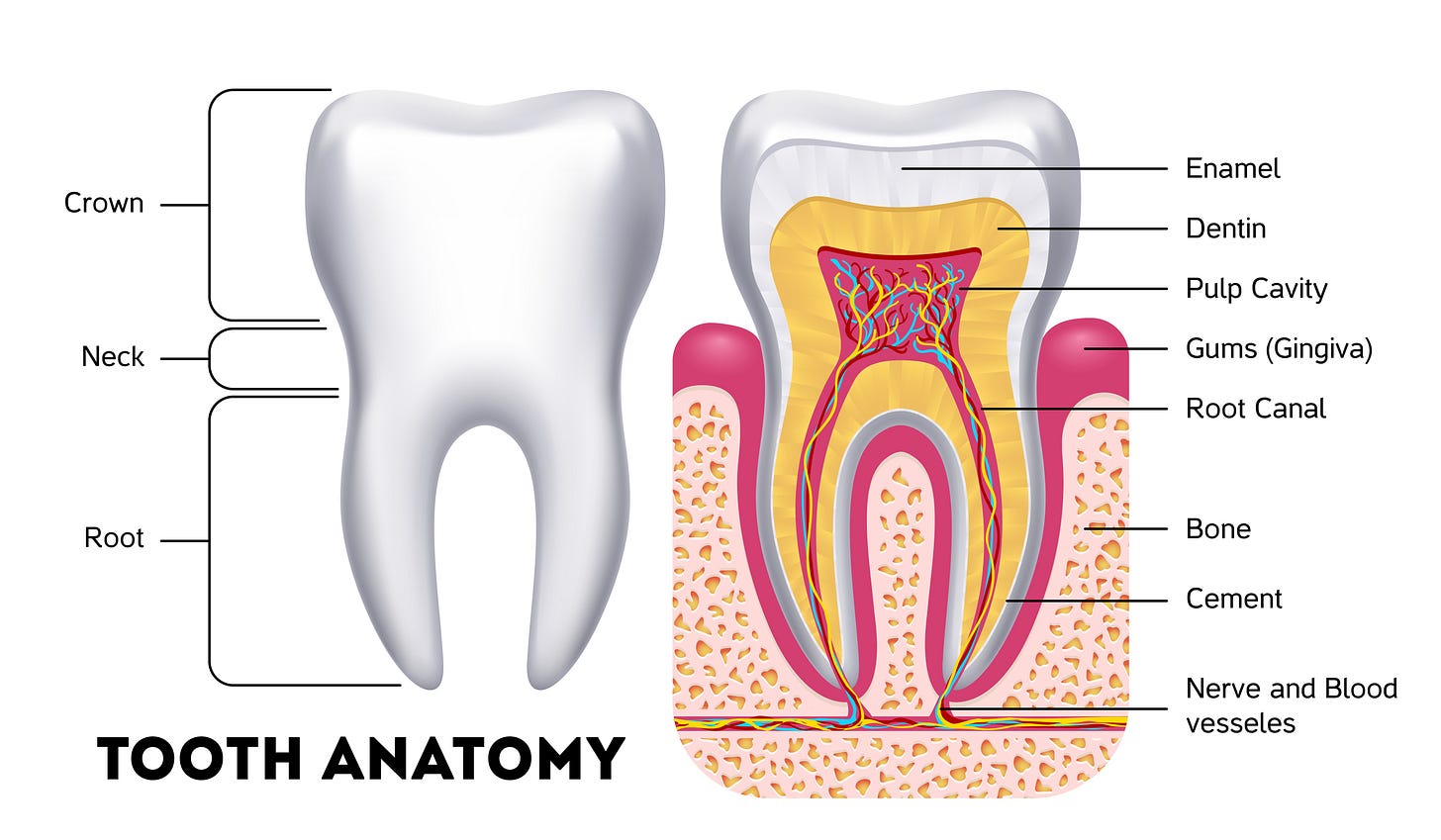
The Tooth That Wouldn’t Heal
Exploring the Biological Realities of Root Canal–Treated Teeth and Their Place in Whole-Body Health
Excerpt
A root canal may eliminate pain and preserve a tooth’s structure, yet from a biological perspective, the tooth is no longer living tissue. In some patients, this devitalized tooth continues to interact with the immune system in ways that standard imaging does not fully reveal. This clinical essay examines what we observe in practice, the limitations of conventional diagnostics, and why thoughtful awareness—not fear—matters when oral health intersects with systemic well-being.
Some health stories don’t begin in the body systems we expect. They begin quietly, in places rarely questioned, and persist until someone looks closer.
The Story That Sparked the Question
Jenny McCarthy reported a period of recurring jaw infections, eyelid growths, and overall decline. Consulting a biological dentist led to a closer evaluation of her long-standing root canal tooth, which was found to be insufficiently cleaned. After further intervention, she experienced meaningful improvement.
This is not presented as causal proof. It is one patient’s narrative. But it is a story that raises an important question: Can a tooth that appears “treated” still affect systemic health?
What a Root Canal Actually Changes
A root canal removes the nerve and blood supply from a tooth to eliminate pain and preserve the structure.
From a biological perspective, however, the tooth is no longer living tissue. It no longer possesses:
Circulation
Immune response
Regenerative capacity
What remains is a structural shell. For many patients, this functions without an immediate clinical issue. For others, the body may continue to respond to the presence of devitalized tissue over time.
What We See Clinically
Two recent examples illustrate a common observation: both teeth showed a darkened, gray appearance upon extraction, quite different from the bone-colored hue of a healthy root. This discoloration often reflects bacterial and/or fungal growth and internal structural changes and dentin dehydration—alterations that are not always apparent on standard radiographs. We also review radiographs (X-rays and CT scans); sometimes pathology is visible in the bone around or beyond the root structure.
These visual findings align with what many clinicians practicing biological dentistry have long noted. They prompt us to look beyond surface-level success metrics.
The Limitation of Imaging Alone
Conventional endodontics has a high success rate in resolving symptoms and preserving teeth. Traditional imaging—mainly periapical (X-ray of the root) radiographs—detects structural breakdown, infection, or major bone loss.
Yet radiographs have inherent limitations. They provide a two-dimensional view of three-dimensional anatomy and may not reveal:
Internal changes within the tooth structure
Microbial activity within dentinal tubules
Subtle, ongoing low-grade immune responses
In other words, a tooth can look “acceptable” on radiographs while still being biologically inactive or harboring complexities beyond the scope of standard imaging. CT scans (CBCT), a three-dimensional view of the tooth and surrounding bone, are helpful in viewing these complexities. Emerging research continues to examine these nuances, such as persistent microbes and fungi even in “well-preformed” canals. In short, even root canals that appear successful in X-rays can still harbor bacteria and fungi that produce waste products and toxins that need to be processed and dealt with.
A Broader View of Health
At Midwest BioHealth, we do not assume all root canal-treated teeth are problems or always neutral. Instead, we ask:
Are there unexplained systemic symptoms without a clear source?
Has every potential contributor—oral and otherwise—been thoughtfully considered?
This approach is not driven by fear but by a need for clinical vigilance. Recognizing these interactions can change how providers assess persistent symptoms and when to recommend additional evaluation or referrals.
Where the Conversation Begins
Stories like Jenny McCarthy’s resonate because they reflect a common patient experience: searching for answers that do not fit neatly into isolated medical or dental silos. Dentistry, in this context, is not separate from the rest of the body. It is part of the larger biological system.
Sometimes the answers patients seek require us to revisit areas long considered “resolved.”
Practical Perspective
A root canal may successfully resolve pain and preserve natural tooth structure—an outcome that remains valuable for many individuals. At the same time, in selected cases, a devitalized tooth may warrant further evaluation when systemic symptoms persist without a clear explanation.
For patients and healthcare colleagues exploring these questions, the following considerations may be helpful:
When symptoms such as unexplained fatigue, joint issues, or chronic inflammation persist despite conventional care, clinicians should recommend a comprehensive oral-systemic assessment. This may include collaboration with biological dentists or additional targeted diagnostics.
Beyond standard radiographs, advanced imaging (such as CBCT when indicated) or clinical evaluation of the tooth’s biological status may reveal more information.
The decision to retain or remove a root canal-treated tooth is always individualized, weighing the desire to preserve structure against the goal of minimizing any potential chronic inflammatory load.
Our role is to guide patients toward a complete understanding of their options. By asking more informed questions and considering the clinical implications of persistent symptoms, providers can recommend targeted diagnostic steps or multidisciplinary care, leading to clearer decisions.
References
(Selected foundational and supporting sources; full bibliography available upon request)
Studies on limitations of periapical radiography in endodontics (e.g., reviews in PMC and Journal of Endodontics highlighting two-dimensional constraints and missed anatomy).
Clinical observations on dentinal tubule microbiology and devitalized teeth (consistent with foundational work in oral biology).
Public accounts from patients such as Jenny McCarthy describing experiences with persistent dental infections (reported in 2025–2026 media).
Broader literature on oral-systemic inflammation pathways (including reviews examining chronic apical periodontitis and host response).
Dr. John Johnson, DDS
Midwest BioHealth
The Johnson Papers